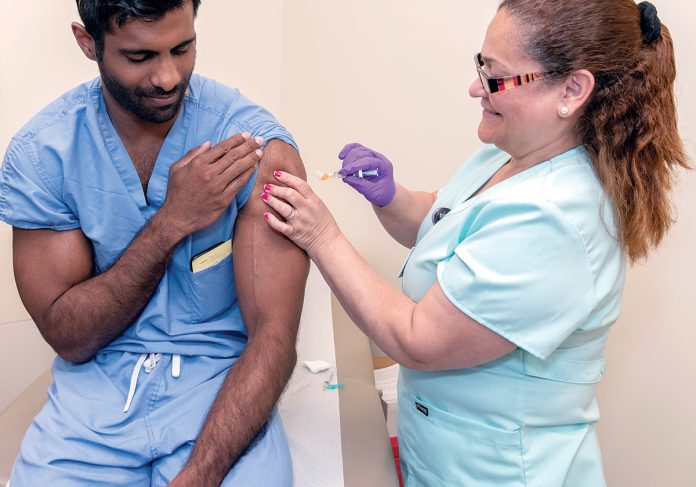
When the nation’s sole yellow-fever vaccine manufacturer paused production in April during a global outbreak, local travelers had one spot for shots, a recurring theme in what the National Center for Biotechnology Information calls the declining inoculation industry.
The yellow-fever virus is transmitted by the Aedes genus of mosquito, which can also carry Zika and dengue fever. Most people infected show no symptoms, but about 15 percent develop the disease, starting with nonspecific symptoms such as fever, chills, nausea and muscle pain. About 20 percent to 50 percent of the people who develop the disease experience a severe case, including severe vomiting, bleeding from the mouth, nose and eyes, jaundice and, ultimately, organ failure of the liver and kidneys, leading to death, according to the Centers for Disease Control and Prevention.
There have been multiple outbreaks in recent years, in Angola and the Democratic Republic of the Congo in 2016, and, most recently, Brazil. About 135 countries require vaccination against the illness before allowing travelers to enter.
Sanofi Pasteur was moving its YF-VAX vaccine production to an updated facility in November 2015 when a manufacturing error eliminated a large number of doses, according to the CDC. Since then, limited production has managed to maintain the national supply, but stock of the vaccine was expected to run out before the 2018 opening of the new U.S. YF-VAX vaccine-manufacturing facility.
The company submitted an expanded-access investigational new drug application to import Stamaril, a yellow-fever vaccine manufactured by Sanofi Pasteur France not licensed in the United States. Due to limited supply, only 250 of the usual 4,000 clinics in the U.S. received Stamaril in April.
Brown Medicine was one of the clinics to receive the vaccine, the only one in Rhode Island. New Englanders with travel plans have since been flocking to the East Providence center to secure their travel requirements.
“I would describe it as just a big strain on the system,” said Dr. Maria Mileno, infectious-disease specialist of the Brown Medicine Travel Clinic, located at 375 Wampanoag Trail. She said paperwork and documentation for the increased number of patients getting inoculated have been a strain on clinic staff. “We’ve been inundated with people needing it.”
Jeffrey Bratberg, clinical professor at the University of Rhode Island’s College of Pharmacy, said the complicated and expensive investment required to produce vaccines, coupled with their low opportunity for profit compared to drug manufacturing, contributes to sluggish investment in vaccine production and monopolized manufacturing of individual vaccines.
“The companies that make vaccines also make drugs and the drugs are more profitable,” Bratberg said.
Whereas drugs are made with nonliving, relatively stable materials, vaccines are created using living organisms, which are much more difficult to store and work with.
“[The vaccine industry has] got two strikes against it,” Bratberg said.
There are no generic vaccines in production, according to “Vaccine Shortages: History, Impact and Prospects for the Future,” published by nonprofit science policy analysis organization Annual Reviews.
Vaccine shortages became a problem in the 2000s, Annual Reviews reports, following 15 years with no shortages. Between 2000 and mid-2005, shortages occurred for vaccines protecting against nine of the 13 diseases for which all children are immunized: diphtheria, influenza, measles, mumps, pertussis, pneumococcal disease, rubella, tetanus and varicella.
The report notes there’s recently been more interest among pharmaceutical companies in reaching new markets than in competing for existing markets of other companies.
“Thus, the United States is vulnerable to single suppliers for the foreseeable future” the report, written in 2006, predicted. Bratberg says that vulnerability remains today.
Vaccine shortages can still happen even where there are competing manufacturers, Bratberg said. For instance, there are two shingles vaccines, Merck’s shingles shot Zostavax and GlaxoSmithKline’s Shingrix. The latter has been recommended as the preferred vaccine for people 50 and older by the CDC, and the resulting demand has contributed to order limits and shipping delays at GlaxoSmithKline, the agency reports.
“There are still efforts that need to be put in place to make it easier to enter existing markets,” Bratberg said. There are two strategies, financial and regulatory, that could encourage more companies to compete in the vaccine industry, he added.
On the financial end, he said, any vaccine that gets development should have first-dollar (without copay applied) reimbursement. On the regulatory side, the U.S. should streamline the vaccine approval process to make it more efficient and faster. That would include providing incentives to develop vaccines for low-volume/high-severity diseases in the form of government funding for development, market exclusivity for other products in exchange for making vaccines to compete in existing markets, tax credits and the waiver of regulatory fees.
Bratberg said the U.S. can also get ahead of vaccine shortages by stockpiling them in sufficient numbers to handle sudden increases in demand and manufacturing problems.