NEW YORK – Cigna Corp.’s proposed deal for Express Scripts Holding Co. faces a drawn-out merger review as the Trump administration’s antitrust enforcers weigh the competitive effects of a wave of consolidation sweeping the health care industry.
The tie-up of the insurer and pharmacy benefit manager comes on the heels of CVS Health Corp.’s agreement to buy insurer Aetna Inc. In both combinations, the companies say they’ll become more efficient firms and help lower health care costs. Whether customers are actually poised to benefit is the key question for antitrust enforcers.
“If Cigna is vying to win share then some of that might be passed through,” Harvard Business School Professor Leemore Dafny said about cost-savings. “The question is how much? How big are those efficiencies, and when they’re done paying all their advisers and themselves, will there be any left over for consumers?”
The challenge for Cigna and CVS will be to convince antitrust enforcers that the answer to that question is yes. The two health care mega-deals come as the Justice Department is rethinking how to approach transactions such as theirs that combine firms operating at different points in an industry supply chain. Such vertical tie-ups don’t raise the same kind of competitive harms that come when direct competitors combine. Yet there are risks that the deals could enable Cigna and CVS to disadvantage rivals.
The Express Scripts deal will probably be reviewed by the Justice Department’s antitrust division rather than the Federal Trade Commission, according to lawyers. The division handles health insurance mergers and successfully blocked Cigna’s sale to Anthem Inc. last year. While the FTC investigates mergers involving PBMs, the Justice Department is investigating the CVS-Aetna deal, which combines an insurer and a PBM.
Consolidation Trend
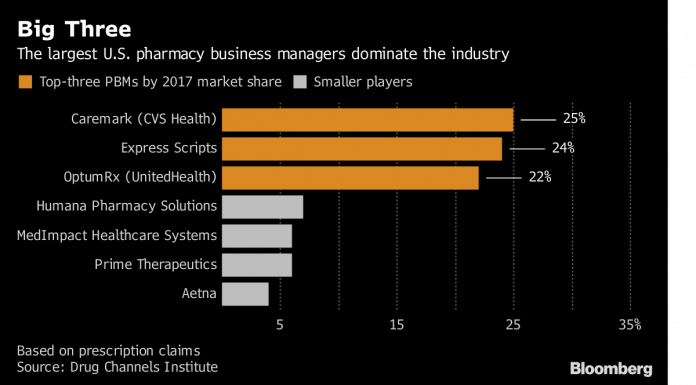
The National Community Pharmacists Association said the Express Scripts deal continues a trend of health care consolidation that has reduced choice for consumers. Express Scripts is the second-biggest pharmacy benefit manager in the U.S. behind CVS’ Caremark business. Along with OptumRx, a unit of UnitedHealth Group Inc., the three PBMs have a combined market share of 70 percent, according to estimates by Drug Channels Institute.
“We’re seeing the growing balkanization of the health care industry, a world in which patients may be forced into a health care kingdom – the CVS-Aetna kingdom, the Cigna-Express Scripts kingdom, the UnitedHealth-OptumRx kingdom, et cetera – where the borders aren’t porous, and patients are stuck with what they get,” B. Douglas Hoey, the head of the group, said in a statement.
The PBMs handle drug benefits for insurers and employers, negotiating prices with drugmakers. They’ve come under particular pressure in recent weeks, with President Donald Trump’s Council of Economic Advisers criticizing the companies’ market power and the opacity of their drug-price contracts.
The tie-up could lead Express Scripts to discriminate against Cigna’s insurer rivals and raise their costs. That could potentially encourage other insurers to form a rival PBM so they don’t have to depend on a combined Cigna-Express Scripts, according to Dafny, who studies health care markets. That would boost competition.
“You could absolutely tell a story where there is heightened competition in both PBMs and insurance segments,” she said. “You could also tell a story where it forecloses some rivals from access to a really important input, and that is excellent PBM services.”
Creating Savings
Fiona Schaeffer, an antitrust lawyer at Milbank, Tweed, Hadley and McCloy in New York, sees the deal creating savings from integrating a pharmacy benefit manager with an insurer. Foreclosing rivals is unlikely given that other insurers such as UnitedHealth have PBMs and continue to serve other insurers, she said.
“It really puts Cigna on the same footing as other major health insurers that already have or are acquiring their own PBM,” she said. “The PBM model is typically one the insurer wants to make available to other insurers, not just to serve themselves.”
Cigna will probably win approval for the takeover from enforcers, Bloomberg Intelligence analyst Jennifer Rie said. Cigna would need market power to effectively discriminate against rivals, but with other large insurers in the market, that risk is less likely, Rie said.
For years, competitive harms from vertical deals have been resolved by putting conditions on how companies operate. But the Justice Department antitrust division under Trump has thrown out that playbook, arguing that behavioral remedies force antitrust enforcers to become regulators who monitor whether companies comply with the conditions. That view prompted the government’s lawsuit against AT&T Inc.’s proposed takeover of Time Warner Inc.
“The Justice Department has made clear its opposition to behavioral remedies,” said Amanda Wait, an antitrust lawyer at Hunton & Williams in Washington, “so that fix is unlikely to win the day for Cigna.”
David McLaughlin is a reporter for Bloomberg News.